Can Your Bladder Rip Again After Month of Your Surgery
| Urinary bladder | |
|---|---|
 ane. Homo urinary system: ii. Kidney, three. Renal pelvis, four. Ureter, 5. Urinary bladder, half dozen. Urethra. (Left side with frontal department) | |
| Details | |
| Precursor | urogenital sinus |
| System | Urinary organization |
| Artery | Superior vesical artery Inferior vesical avenue Umbilical artery Vaginal artery |
| Vein | Vesical venous plexus |
| Nerve | Vesical nervous plexus |
| Identifiers | |
| Latin | vesica urinaria |
| MeSH | D001743 |
| TA98 | A08.3.01.001 |
| TA2 | 3401 |
| FMA | 15900 |
| Anatomical terminology [edit on Wikidata] | |
The urinary bladder, or simply bladder, is a hollow organ in humans and other vertebrates that stores urine from the kidneys before disposal past urination. In humans the bladder is a distensible organ that sits on the pelvic flooring. Urine enters the bladder via the ureters and exits via the urethra. The typical human float volition agree between 300 and 500 ml (10.14 and sixteen.91 fl oz) earlier the urge to empty occurs, but tin hold considerably more.[1] [2]
The Latin phrase for "urinary bladder" is vesica urinaria, and the term vesical or prefix vesico - appear in connection with associated structures such as vesical veins. The modernistic Latin word for "bladder" – cystis – appears in associated terms such equally cystitis (inflammation of the float).
Structure [edit]

Male and female urinary bladders in lateral cantankerous-section
In humans, the bladder is a hollow muscular organ situated at the base of the pelvis. In gross anatomy, the bladder can be divided into a wide fundus, a body, an noon, and a neck.[3] The apex is directed forrad toward the upper part of the pubic symphysis, and from there the median umbilical ligament continues upward on the back of the anterior intestinal wall to the umbilicus. The peritoneum is carried past it from the apex on to the abdominal wall to form the eye umbilical fold. The cervix of the bladder is the area at the base of operations of the trigone that surrounds the internal urethral orifice that leads to the urethra.[3] In males the cervix of the urinary bladder is side by side to the prostate gland.
The bladder has 3 openings. The two ureters enter the bladder at ureteric orifices, and the urethra enters at the trigone of the bladder. These ureteric openings have mucosal flaps in front of them that human activity as valves in preventing the backflow of urine into the ureters,[iv] known as vesicoureteral reflux. Betwixt the ii ureteric openings is a raised area of tissue chosen the interureteric crest.[3] This makes the upper boundary of the trigone. The trigone is an area of smooth musculus that forms the floor of the bladder higher up the urethra.[five] Information technology is an area of smooth tissue for the easy flow of urine into and from this office of the bladder - in contrast to the irregular surface formed by the rugae.
The walls of the bladder take a series of ridges, thick mucosal folds known as rugae that allow for the expansion of the bladder. The detrusor muscle is the muscular layer of the wall made of smooth muscle fibers bundled in spiral, longitudinal, and round bundles.[6] The detrusor musculus is able to change its length. It tin also contract for a long time whilst voiding, and it stays relaxed whilst the bladder is filling.[7] The wall of the urinary bladder is commonly iii–5 mm thick.[8] When well distended, the wall is normally less than 3 mm.
Nearby structures [edit]

Bladder location and associated structures in the male
In men, the prostate gland lies outside the opening for the urethra. The middle lobe of the prostate causes an peak in the mucous membrane behind the internal urethral orifice called the uvula of urinary bladder. The uvula can enlarge when the prostate becomes enlarged.
The bladder is located below the peritoneal cavity about the pelvic floor and behind the pubic symphysis. In men, information technology lies in front of the rectum, separated past the recto-vesical pouch, and is supported past fibres of the levator ani and of the prostate gland. In women, it lies in front of the uterus, separated by the vesico-uterine pouch, and is supported by the lift ani and the upper part of the vagina.[eight]
Blood and lymph supply [edit]
The bladder receives blood by the vesical arteries and drained into a network of vesical veins.[ix] The superior vesical avenue supplies blood to the upper part of the bladder. The lower part of the bladder is supplied by the inferior vesical artery, both of which are branches of the internal iliac arteries.[9] In females, the uterine and vaginal arteries provide additional blood supply.[9] Venous drainage begins in a network of small vessels on the lower lateral surfaces of the bladder, which coalesce and travel with the lateral ligaments of the float into the internal iliac veins.[9]
The lymph drained from the bladder begins in a serial of networks throughout the mucosal, muscular and serosal layers. These so form 3 sets of vessels: ane set about the trigone draining the bottom of the bladder; ane set draining the superlative of the bladder; and another gear up draining the outer undersurface of the bladder. The bulk of these vessels drain into the external iliac lymph nodes.[nine]
Nerve supply [edit]
The float receives both sensory and motor supply from sympathetic and the parasympathetic nervous systems.[9] The motor supply from both sympathetic fibers, most of which arise from the superior and inferior hypogastric plexuses and fretfulness, and from parasympathetic fibers, which come from the pelvic splanchnic nerves.[10]
Awareness from the bladder, relating to amplification or to irritation (such every bit by infection or a stone) is transmitted primarily through the parasympathetic nervous organisation.[9] These travel via sacral nerves to S2-iv.[11] From hither, sensation travels to the encephalon via the dorsal columns in the spinal cord.[ix]
Microanatomy [edit]
When viewed nether a microscope the bladder tin be seen to accept an inner lining (called epithelium), 3 layers of musculus fibres, and an outer adventitia.[half-dozen]
The inner wall of the bladder is called urothelium, a type of transitional epithelium formed by three to six layers of cells; the cells may become more cuboidal or flatter depending on whether the bladder is empty or full.[vi] Additionally, these are lined with a mucous membrane consisting of a surface glycocalyx that protects the cells beneath information technology from urine.[12] The epithelium lies on a thin basement membrane, and a lamina propria.[6] The mucosal lining also offers a urothelial barrier against the passing of infections.[thirteen]
These layers are surrounded past iii layers of musculus fibres bundled every bit an inner layer of fibres orientated longitudinally, a heart layer of circular fibres, and an outermost layer of longitudinal fibres; these form the detrusor muscle, which can exist seen with the naked centre.[6]
The exterior of the bladder is protected by a serous membrane called adventitia.[6] [xiv]
-
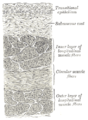
Vertical section of bladder wall
-
Layers of the urinary bladder wall and cross-section of the detrusor muscle
-
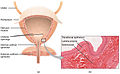
Beefcake of the male person bladder, showing transitional epithelium and office of the wall in a histological cut-out
Development [edit]
In the developing embryo, at the hind stop lies a cloaca. This, over the fourth to the seventh week, divides into a urogenital sinus and the beginnings of the anal canal, with a wall forming betwixt these ii inpouchings called the urorectal septum.[15] The urogenital sinus divides into three parts, with the upper and largest part becoming the bladder; the heart part condign the urethra, and the lower role changes depending on the biological sex of the embryo.[15]
The homo urinary bladder derives from the urogenital sinus, and it is initially continuous with the allantois. The upper and lower parts of the float develop separately and bring together together around the middle role of evolution.[5] At this fourth dimension the ureters motility from the mesonephric ducts to the trigone.[five] In males, the base of the bladder lies betwixt the rectum and the pubic symphysis. It is superior to the prostate, and separated from the rectum past the recto-vesical pouch. In females, the float sits inferior to the uterus and anterior to the vagina; thus its maximum capacity is lower than in males. Information technology is separated from the uterus by the vesico-uterine pouch. In infants and young children the urinary bladder is in the belly even when empty.[16]
Function [edit]
Urine, excreted by the kidneys, collects in the bladder because of drainage from two ureters, earlier disposal by urination (micturition).[11] Urine leaves the float via the urethra, a single muscular tube ending in an opening called the urinary meatus, where it exits the body.[9] Urination involves coordinated musculus changes involving a reflex based in the spine, with higher inputs from the brain.[xi] During urination, the detrusor muscle contracts, and the external urinary sphincter and muscles of the perineum relax, allowing urine to pass through the urethra and out of the body.[11]
The urge to pass urine stems from stretch receptors that actuate when between 300 - 400 mL urine is held within the bladder.[11] As urine accumulates, the rugae flatten and the wall of the bladder thins as it stretches, allowing the bladder to store larger amounts of urine without a pregnant ascension in internal pressure.[17] Urination is controlled by the pontine micturition middle in the brainstem.[18]
Stretch receptors in the float indicate the parasympathetic nervous organization to stimulate the muscarinic receptors in the detrusor to contract the muscle when the float is distended.[xix] This encourages the bladder to miscarry urine through the urethra. The principal receptor activated is the M3 receptor, although M2 receptors are also involved and whilst outnumbering the M3 receptors they are not then responsive.[20]
The main relaxant pathway is via the adenylyl cyclase cAMP pathway, activated via the β3 adrenergic receptors. The β2 adrenergic receptors are also present in the detrusor and even outnumber β3 receptors, but they do not take as of import an result in relaxing the detrusor shine muscle.[7] [21] [22]
Clinical significance [edit]
Inflammation and infection [edit]

Cystitis refers to infection or inflammation of the bladder. It unremarkably occurs equally part of a urinary tract infection.[23] In adults, it is more common in women than men, owing to a shorter urethra. Information technology is common in males during babyhood, and in older men where an enlarged prostate may cause urinary retention.[23] Other risk factors include other causes of blockage or narrowing, such as prostate cancer or the presence of vesico-ureteric reflux; the presence of outside structures in the urinary tract, such equally urinary catheters; and neurologic problems that make passing urine difficult.[23] Infections that involve the float can cause pain in the lower belly (above the pubic symphysis, so chosen "suprapubic" pain), particularly before and afterward passing urine, and a desire to pass urine oft and with little alert (urinary urgency).[23] Infections are ordinarily due to bacteria, of which the nigh common is E coli.[23]
When a urinary tract infection or cystitis is suspected, a medical practitioner may asking a urine sample. A dipstick placed in the urine may be used to see if the urine has white blood cells, or the presence of nitrates which may indicate an infection. The urine specimen may be also sent for microbial civilization and sensitivity to assess if a particular leaner grows in the urine, and identify its antibody sensitivities.[23] Sometimes, additional investigations may be requested. These might include testing the function of the kidneys by assessing electrolytes and creatinine; investigating for blockages or narrowing of the renal tract with a ultrasound, and testing for an enlarged prostate with a digital rectal examination.[23]
Urinary tract infections or cystitis are treated with antibiotics, many of which are consumed by oral cavity. Serious infections may require treatment with intravenous antibiotics.[23]
Interstitial cystitis refers to a condition in which the bladder is infected due to a cause that is not bacteria.[24] [ citation needed ]
Incontinence and retention [edit]
Frequent urination can be due to excessive urine product, small bladder capacity, irritability or incomplete emptying. Males with an enlarged prostate urinate more than oftentimes. One definition of an overactive bladder is when a person urinates more than eight times per day.[25] An overactive float can ofttimes cause urinary incontinence. Though both urinary frequency and volumes have been shown to have a circadian rhythm, significant day and dark cycles,[26] it is not entirely articulate how these are disturbed in the overactive bladder. Urodynamic testing tin can assistance to explain the symptoms. An underactive bladder is the status where there is a difficulty in passing urine and is the main symptom of a neurogenic bladder. Frequent urination at night may signal the presence of bladder stones.
Disorders of or related to the bladder include:
- Float exstrophy
- Bladder sphincter dyssynergia, a condition in which the sufferer cannot coordinate relaxation of the urethra sphincter with the contraction of the bladder muscles
- Paruresis
- Trigonitis
- Underactive bladder, a condition with its main symptom being urinary retention.[27]
Disorders of bladder role may be dealt with surgically, by re-directing the menstruation of urine or by replacement with an bogus urinary bladder. The book of the bladder may exist increased by float augmentation. An obstruction of the float neck may exist astringent enough to warrant surgery.
Cancer [edit]

Cancer of the bladder is known as bladder cancer. It is usually due to cancer of the urothelium, the cells that line the surface of the bladder. Bladder cancer is more common after the historic period of 40, and more common in men than women;[28] other risk factors include smoking and exposure to dyes such every bit effluvious amines and aldehydes.[28] When cancer is nowadays, the near mutual symptom in an affected person is claret in the urine; a concrete medical examination may be otherwise normal, except in late disease.[28] Bladder cancer is near frequently due to cancer of the cells lining the ureter, called transitional cell carcinoma, although it can more rarely occur as a squamous cell carcinoma if the blazon of cells lining the urethra have inverse due to chronic inflammation, such as due to stones or schistosomiasis.[28]
Investigations performed unremarkably include collecting a sample of urine for an inspection for malignant cells nether a microscope, called cytology, as well equally medical imaging by a CT urogram or ultrasound.[28] If a apropos lesion is seen, a flexible camera may be inserted into the float, called cystoscopy, in order to view the lesion and take a biopsy, and a CT scan will exist performed of other torso parts (a CT scan of the chest, abdomen and pelvis) to look for additional metastatic lesions.[28]
Treatment depends on the cancer's stage. Cancer present only in the bladder may be removed surgically via cystoscopy; an injection of the chemotherapeutic mitomycin C may exist performed at the aforementioned time.[28] Cancers that are high form may exist treated with an injection of the BCG vaccine into the bladder wall, and may require surgical removal if it does not resolve.[28] Cancer that is invading through the bladder wall may be managed past complete surgical removal of the bladder (radical cystectomy), with the ureters diverted into a segment of function of ileum connected to a stoma pocketbook on the skin.[28] Prognosis can vary markedly depending on the cancer's stage and course, with a better prognosis associated with tumours plant only in the float, that are low form, that don't invade through the bladder wall, and that is papillary in visual appearance.[28]
Investigation [edit]


A number of investigations are used to examine the float. The investigations that are ordered will depend on the taking of a medical history and an examination. The examination may involve a medical practitioner feeling in the suprapubic surface area for tenderness or fullness that might betoken an inflamed or full bladder.[ citation needed ] Claret tests may be ordered that may betoken inflammation; for example a full claret count may demonstrate elevated white blood cells, or a C-reactive protein may be elevated in an infection.[ commendation needed ]
Some forms of medical imaging exist to visualise the bladder. A bladder ultrasound may exist conducted to view how much urine is within the bladder, indicating urinary memory. A urinary tract ultrasound, conducted past a more trained operator, may be conducted to view whether there are stones, tumours or sites of obstacle within the float and urinary tract. A CT scan may as well exist ordered.
A flexible internal camera, called a cystoscope, can be inserted to view the internal appearance of the bladder and take a biopsy if required.
Urodynamic testing can help to explain the symptoms.
Other animals [edit]
Mammals [edit]
All mammals have a urinary bladder. This construction begins as an embryonic cloaca. In the vast majority, this eventually becomes differentiated into a dorsal part connected to the intestine and a ventral part which becomes associated with the urinogenital passage and urinary bladder. The only mammals in which this does non have place are the platypus and the spiny anteater both of which retain the cloaca into adulthood.[29]
The mammalian bladder is an organ that regularly stores a hyperosmotic concentration of urine. It therefore is relatively impermeable and has multiple epithelial layers. The urinary float of the cetaceans (whales and dolphins) is proportionally smaller than that of land-dwelling mammals.[xxx]
Reptiles [edit]
In all reptiles, the urinogenital ducts and the anus both empty into an organ called a cloaca. In some reptiles, a midventral wall in the cloaca may open into a urinary float, only not all. It is nowadays in all turtles and tortoises besides as most lizards but is defective in the monitor cadger, the legless lizards. It is absent in the snakes, alligators, and crocodiles.[29] : p. 474
Many turtles, tortoises, and lizards have proportionally very big bladders. Charles Darwin noted that the Galapagos tortoise had a float which could store up to 20% of its body weight.[31] Such adaptations are the result of environments such equally remote islands and deserts where water is very deficient.[32] Other desert-dwelling reptiles have big bladders that can store a long-term reservoir of water for upward to several months and aid in osmoregulation.[33]
Turtles have two or more than accompaniment urinary bladders, located lateral to the neck of the urinary float and dorsal to the pubis, occupying a significant portion of their body crenel.[34] Their bladder is also usually bilobed with a left and correct department. The right section is located under the liver, which prevents large stones from remaining in that side while the left section is more than likely to have calculi.[35]
Amphibians [edit]
Most aquatic and semi-aquatic amphibians have a membranous skin which allows them to absorb water directly through information technology. Some semi-aquatic animals also take similarly permeable bladder membrane.[36] As a result, they tend to accept high rates of urine production to offset this high water intake, and have urine which is low in dissolved salts. The urinary bladder assists such animals to retain salts. Some aquatic amphibian such as Xenopus practise not reabsorb h2o, to prevent excessive water influx.[37] For land-home amphibians, dehydration results in reduced urine output.[38]
The amphibian float is normally highly distensible and among some land-abode species of frogs and salamanders may account for betwixt twenty% and 50% of their total body weight.[38]
Fish [edit]
The gills of almost teleost fish aid to eliminate ammonia from the body, and fish alive surrounded by water, but most all the same accept a distinct float for storing waste fluid. The urinary float of teleosts is permeable to water, though this is less truthful for freshwater dwelling species than saltwater species.[31] : p. 219 Near fish also take an organ called a swim-bladder which is unrelated to the urinary bladder except in its membranous nature. The loaches, pilchards, and herrings are among the few types of fish in which a urinary bladder is poorly developed. It is largest in those fish which lack an air bladder, and is situated in front of the oviducts and behind the rectum.[39]
Birds [edit]
In well-nigh all bird species, there is no urinary float per se.[twoscore] Although all birds have kidneys, the ureters open direct into a cloaca which serves every bit a reservoir for urine, fecal affair, and eggs.[41]
Crustaceans [edit]
Unlike the urinary bladder of vertebrates, the urinary bladder of crustaceans both stores and modifies urine.[42] The bladder consists of two sets of lateral and central lobes. The cardinal lobes sit down almost the digestive organs and the lateral lobes extend along the front and sides of the crustacean's body cavity.[42] The tissue of the bladder is sparse epithelium.[42]
See also [edit]
- Blastoff blocker
- Cystitis glandularis
- UPK1B
References [edit]
- ^ Boron, Walter F.; Boulpaep, Emile L. (2016). Medical Physiology. 3: Elsevier Health Sciences. p. 738. ISBN9781455733286 . Retrieved 1 June 2016.
{{cite book}}: CS1 maint: location (link) - ^ Walker-Smith, John; Murch, Simon (1999). Cardozo, Linda (ed.). Diseases of the Pocket-size Intestine in Childhood (4 ed.). CRC Press. p. sixteen. ISBN9781901865059 . Retrieved 1 June 2016.
- ^ a b c Netter, Frank H. (2014). Atlas of Man Anatomy Including Student Consult Interactive Ancillaries and Guides (6th ed.). Philadelphia, Penn.: West B Saunders Co. pp. 346–8. ISBN978-14557-0418-7.
- ^ "SEER Training:Urinary Bladder". preparation.seer.cancer.gov.
- ^ a b c Viana R, Batourina Eastward, Huang H, Dressler GR, Kobayashi A, Behringer RR, Shapiro E, Hensle T, Lambert S, Mendelsohn C (October 2007). "The development of the bladder trigone, the center of the anti-reflux machinery". Development. 134 (20): 3763–9. doi:x.1242/dev.011270. PMID 17881488.
- ^ a b c d e f Young, Barbara; O'Dowd, Geraldine; Woodford, Phillip (2013). "Urinary system". Wheater'due south functional histology: a text and colour atlas (6th ed.). Philadelphia: Elsevier. pp. 315–7. ISBN9780702047473.
- ^ a b Andersson KE, Arner A (July 2004). "Urinary bladder contraction and relaxation: physiology and pathophysiology". Physiol. Rev. 84 (3): 935–86. CiteSeerX10.1.1.324.7009. doi:ten.1152/physrev.00038.2003. PMID 15269341.
- ^ a b Page 12 in: Uday Patel (2010). Imaging and Urodynamics of the Lower Urinary Tract. Springer Science & Business Media. ISBN9781848828360.
- ^ a b c d e f g h i Standring, Susan, ed. (2016). "Urinary bladder". Gray'south anatomy : the anatomical basis of clinical practice (41st ed.). Philadelphia. pp. 1255–1261. ISBN9780702052309. OCLC 920806541.
- ^ Moore, Keith; Anne Agur (2007). Essential Clinical Beefcake, Third Edition. Lippincott Williams & Wilkins. pp. 227–228. ISBN978-0-7817-6274-8.
- ^ a b c d due east Barrett, Kim E; Barman, Susan Thou; Yuan, Jason X-J; Brooks, Heddwen (2019). "37. Renal function & Micturition: The Bladder". Ganong's review of medical physiology (26th ed.). New York. pp. 681–682. ISBN9781260122404. OCLC 1076268769.
- ^ Stromberga, Z; Chess-Williams, R; Moro, C (seven March 2019). "Histamine modulation of urinary bladder urothelium, lamina propria and detrusor contractile action via H1 and H2 receptors". Scientific Reports. 9 (1): 3899. Bibcode:2019NatSR...nine.3899S. doi:10.1038/s41598-019-40384-1. PMC6405771. PMID 30846750.
- ^ Janssen, DA (January 2013). "The distribution and function of chondroitin sulfate and other sulfated glycosaminoglycans in the human bladder and their contribution to the protective bladder barrier". The Journal of Urology. 189 (1): 336–42. doi:x.1016/j.juro.2012.09.022. PMID 23174248.
- ^ Fry, CH; Vahabi, B (Oct 2016). "The Office of the Mucosa in Normal and Abnormal Bladder Function". Basic & Clinical Pharmacology & Toxicology. 119 Suppl three: 57–62. doi:10.1111/bcpt.12626. PMC5555362. PMID 27228303.
- ^ a b Sadley, TW (2019). "Bladder and urethra". Langman's medical embryology (14th ed.). Philadelphia: Wolters Kluwer. pp. 263–66. ISBN9781496383907.
- ^ Moore, Keith L.; Dalley, Arthur F (2006). Clinically Oriented Anatomy (5th ed.). Lippincott Williams & Wilkins. ISBN9780781736398.
- ^ Marieb, Mallatt. "23". Human Anatomy (fifth ed.). Pearson International. p. 700.
- ^ Purves, Dale (2011). Neuroscience (5. ed.). Sunderland, Mass.: Sinauer. p. 471. ISBN978-0-87893-695-3.
- ^ Giglio, D; Tobin, M (2009). "Muscarinic receptor subtypes in the lower urinary tract". Pharmacology. 83 (5): 259–69. doi:ten.1159/000209255. PMID 19295256.
- ^ Uchiyama, T; Chess-Williams, R (Dec 2004). "Muscarinic receptor subtypes of the bladder and alimentary canal". Journal of Polish Muscle Inquiry = Nihon Heikatsukin Gakkai Kikanshi. 40 (vi): 237–47. doi:10.1540/jsmr.40.237. PMID 15725706.
- ^ Moro, Christian; Tajouri, Lotti; Chess-Williams, Russ (2013). "Adrenoceptor Function and Expression in Bladder Urothelium and Lamina Propria". Urology. 81 (i): 211.e1–211.e7. doi:10.1016/j.urology.2012.09.011. PMID 23200975.
- ^ Chancellor, Thousand. B.; Yoshimura, N. (2004). "Neurophysiology of Stress Urinary Incontinence". Rev. Urol. 6 Suppl iii: S19–28. PMC1472861. PMID 16985861.
- ^ a b c d e f g h Davidson'southward 2018, pp. 426–429.
- ^ "Interstitial cystitis". Mayo Clinic. 14 September 2019. Retrieved x May 2020.
- ^ "Overactive Bladder". Cornell Medical College. Archived from the original on 2 June 2016. Retrieved 21 August 2013.
- ^ Negoro, Hiromitsu (2012). "Involvement of urinary float Connexin43 and the circadian clock in coordination of diurnal micturition rhythm". Nature Communications. three: 809. Bibcode:2012NatCo...iii..809N. doi:10.1038/ncomms1812. PMC3541943. PMID 22549838.
- ^ C, Moro; C, Phelps; V, Veer; J, Clark; P, Glasziou; Kao, Tikkinen; Am, Scott (24 Nov 2021). "The effectiveness of parasympathomimetics for treating underactive float: A systematic review and meta-analysis". Neurourology and urodynamics. doi:10.1002/nau.24839. ISSN 1520-6777. PMID 34816481.
- ^ a b c d e f g h i j Ralston, Stuart H.; Penman, Ian D.; Strachan, Mark Due west.; Hobson, Richard P. (eds.) (2018). "Urothelial tumours". Davidson'south principles and practice of medicine (23rd ed.). Elsevier. pp. 435–six. ISBN978-0-7020-7028-0.
- ^ a b Herbert Westward. Rand (1950). The Chordates. Balkiston.
- ^ John Hunter (26 March 2015). The Works of John Hunter, F.R.Due south. Cambridge Academy. p. 35. ISBN978-1-108-07960-0.
- ^ a b P.J. Bentley (14 March 2013). Endocrines and Osmoregulation: A Comparative Account in Vertebrates. Springer Science & Business Media. ISBN978-3-662-05014-ix.
- ^ Paré, Jean (eleven January 2006). "Reptile Basics: Clinical Anatomy 101" (PDF). Proceedings of the N American Veterinary Conference. 20: 1657–1660.
- ^ Davis, Jon R.; DeNardo, Dale F. (15 April 2007). "The urinary bladder as a physiological reservoir that moderates dehydration in a large desert cadger, the Gila monster Heloderma suspectum". Journal of Experimental Biology. 210 (8): 1472–1480. doi:ten.1242/jeb.003061. ISSN 0022-0949. PMID 17401130.
- ^ Wyneken, Jeanette; Witherington, Dawn (February 2015). "Urogenital System" (PDF). Anatomy of Sea Turtles. 1: 153–165.
- ^ Defined, Stephen J.; Mader, Douglas R. (2005). Reptile Medicine and Surgery. Amsterdam: Elsevier Wellness Sciences. pp. 481, 597. ISBN9781416064770.
- ^ Urakabe, Shigeharu; Shirai, Dairoku; Yuasa, Shigekazu; Kimura, Genjiro; Orita, Yoshimasa; Abe, Hiroshi (1976). "Comparative study of the effects of unlike diuretics on the permeability properties of the toad bladder". Comparative Biochemistry and Physiology Office C: Comparative Pharmacology. 53 (ii): 115–119. doi:ten.1016/0306-4492(76)90063-0. PMID 5237.
- ^ Shibata, Yuki; Katayama, Izumi; Nakakura, Takashi; Ogushi, Yuji; Okada, Reiko; Tanaka, Shigeyasu; Suzuki, Masakazu (2015). "Molecular and cellular characterization of urinary bladder-type aquaporin in Xenopus laevis". General and Comparative Endocrinology. 222: 11–xix. doi:10.1016/j.ygcen.2014.09.001. PMID 25220852.
- ^ a b Laurie J. Vitt; Janalee P. Caldwell (25 March 2013). Herpetology: An Introductory Biology of Amphibians and Reptiles. Academic. p. 184. ISBN978-0-12-386920-3.
- ^ Owen, Richard (1843). Lectures on the comparative anatomy and physiology of the invertebrate animals. London: Longman, Brown, Green, and Longmans. pp. 283–284.
- ^ Cornell University. Laboratory of Ornithology (xix September 2016). Handbook of Bird Biology. John Wiley & Sons. ISBN978-1-118-29105-4.
- ^ Charles Knight (1854). The English Cyclopaedia: A New Dictionary of Universal Cognition. Bradbury and Evans. p. 136.
- ^ a b c Nonmammalian animal models for biomedical inquiry. Woodhead, Avril D. Boca Raton, Fla.: CRC Printing. 1989. pp. 51–52. ISBN0-8493-4763-7. OCLC 18816053.
{{cite book}}: CS1 maint: others (link)
- Books
- editor-in-main, Susan Standring; department editors, Neil R. Borley et al., ed. (2008). Gray's beefcake : the anatomical basis of clinical do (40th ed.). London: Churchill Livingstone. ISBN978-0-8089-2371-8.
- Ralston, Stuart H.; Penman, Ian D.; Strachan, Mark W.; Hobson, Richard P. (eds.) (2018). Davidson's principles and exercise of medicine (23rd ed.). Elsevier. ISBN978-0-7020-7028-0.
External links [edit]
- Beefcake photograph: Urinary/mammal/bladder/bladder1 - Comparative Organology at Academy of California, Davis – "Mammal, bladder (LM, Medium)"
- Bladder (ISSN 2327-2120) – An open-access journal on float biology and diseases.
Source: https://en.wikipedia.org/wiki/Urinary_bladder

แสดงความคิดเห็น for "Can Your Bladder Rip Again After Month of Your Surgery"